Panama: Communities in Action to End Health Inequality for All
by UNDP Latin America and the Caribbean | Original article published on 1 December 2021
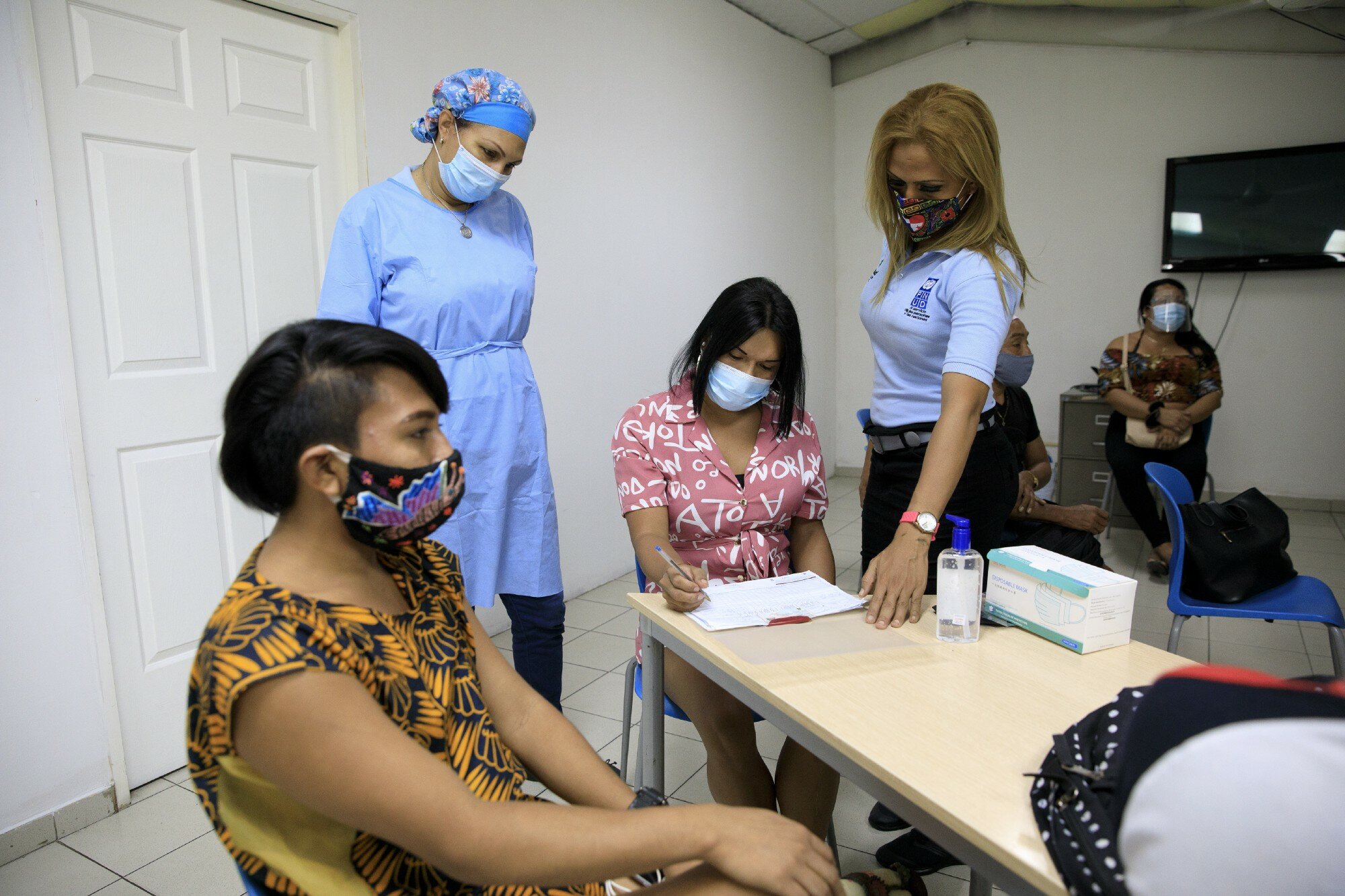
Leanis Zuñiga to the right, community outreach worker, at Viviendo Positivamente supporting one of her clients. Photo by UNDP
The new Global AIDS Strategy 2021–2026 — End Inequalities. End AIDS aims to reduce the inequalities that drive the AIDS epidemic and prioritize people who are not yet accessing life-saving human immunodeficiency virus (HIV) services.
On this World AIDS Day, we celebrate the efforts of countries in Latin America and the Caribbean to close the gaps that are preventing progress towards ending AIDS. In the region, we highlight the case of Panama which shows how the approach of ‘social contracting’ can address inequalities, and ensure services are provided to key and vulnerable populations.
Since 2003, the Global Fund to Fight AIDS, Tuberculosis and Malaria has provided grants to the country to help strengthen its systems for and health and increase access to HIV and Tuberculosis services for those most in need. The work of the Global Fund with the United Nations Development Programme (UNDP), the government, and local partner organizations have resulted in over 12,800 people now accessing anti-retroviral treatment and 18,800 people receiving counseling and testing
Due to its income classification, Panama will not be eligible for Global Fund financing from January 2022. It was therefore imperative to ensure that essential services for key populations (gay men and other men having sex with men, sex workers, transgender people, people who use drugs and people in prison and other closed settings), which tend to be disproportionately affected by health inequalities, can continue uninterrupted into the future.
Civil society organizations (CSOs) and social contracting
In Panama and other countries, CSOs play a vital role in reaching the key population groups most vulnerable to HIV and TB, by providing them with and connecting them to prevention, treatment, and care services, advocating for their rights, and addressing barriers associated with stigma and discrimination.
Social contracting is the process whereby CSOs receive government funding to deliver health prevention, treatment, care, and support services. This role becomes even more important as Panama moves towards domestically financed programmes.
Experience has shown that CSOs can often reach where the state health system cannot. As groups comprised of key populations themselves, CSOs have an intimate understanding of the forces of exclusion that prevent access to services. They are uniquely positioned to reach those pushed to the margins of society. Having already built long-term relationships within communities, CSOs can conduct outreach by going directly to the people who need help the most, who are sometimes most accessible by those in their peer group.
“The advantage of civil society organizations is that these are peer organizations for key populations. This makes it easier to overcome discrimination-based barriers and create greater openings for key populations to access health care services.”
Dr. Jairo Osorio, working with the Ministry of Health of Panama.
In 2017, the UNDP carried out a review to determine if Panama was ready to continue providing services via social contracting after the end of the Global Fund grant. The review underlined the need to scale up the system of public financing for CSOs if critical services were to continue to be delivered to key populations after 2021.
The work which followed, led by the UNDP, was geared towards building the framework for social contracting. It was a complex task, involving a series of consultation processes, and rigorous examination of Panama’s legal, policy and financing mechanisms, as well as other aspects, including how the performance of CSOs could be monitored and evaluated, which is essential to ensure accountability and value for money.
Getting ‘buy-in’ from all parties and stakeholders in the process was essential because decades of experience in international development have demonstrated that top-down solutions tend to fail in the long term. Mutual trust and openness to new ways of interfacing between government and CSOs are essential to a successful outcome. For the Panama Ministry of Health, this meant embracing a different funding structure and level of responsibility in its engagement with CSOs. For CSOs themselves, it meant ensuring they were prepared to comply with government regulations for receiving public funding.
An important aspect of ensuring successful social contracting is working with CSOs to develop their ability to bid successfully to work with the government. This is often referred to as ‘capacity building’, one area where UNDP brings the strongest expertise and experience. A few of the areas where CSOs may need assistance include having the necessary human resources to coordinate a project, having effective financial monitoring functions, or having sufficient knowledge of administrative processes in government ministries.
“It is not easy for one or two organizations to be a spokesperson on these issues. We need to come together as one voice.”
Ricardo Beteta, president of AHMNP, the first legally recognized LGBTI organization in Panama.
For people living with HIV in Panama, the continued provision of services is literally a lifeline. The transition from the Global Fund to domestic financing is a vital step in ensuring that these services can future continue. With this work, Panama is one step closer to ending health inequality for all.
Retrieved from https://pnudlac.medium.com/panama-communities-in-action-to-end-health-inequality-for-all-cb3ad11ba7d8